Pathways early intervention program for toddlers with autism
Pamela Rosenthal Rollins*
University of Texas at Dallas, Callier Center for Communication Disorders, 1966 Inwood Road, Dallas, USA
Abstract
Early identification and intervention that focus on the core social deficits of children with autism spectrum disorder (ASD) are imperative for these children to be able to reach their optimal potential. This report examines the Pathways Early Autism Intervention (Pathways), a translational parent-mediated, naturalistic developmental behavioral intervention (NDBI) for toddlers with ASD. Pathways fits the service delivery model and principles of Texas’ state-funded Early Childhood Intervention (ECI) programs. Pathways was found to be more effective than traditional ECI programs in improving early foundational social communication skills and in reducing parental stress in culturally and economically diverse toddlers with ASD. Pathways shows promise as an effective ASD specific intervention with the potential of being implemented within publicly funded ECI programs.
Intriduction
Autism spectrum disorder (ASD) is a complex, heterogeneous neurodevelopmental disorder that severely compromises the development of social relatedness, reciprocity, and social communication. The Centers for Disease Control and Prevention estimates that 1 in 68 children are on the autism spectrum, which represents a twenty-fold increase since the early 1990s1. As a result of heightened societal awareness, there has been substantial growth in research that advances our understanding of the genetic, neurobiological, and developmental underpinnings of the disorder. This has led to improvements in behavioral markers for early detection and recommendations for treatment strategies. Although there is still no cure for ASD, early identification and intervention can make a significant difference in a child’s IQ, communication, and adaptive functioning2-5.
Nonetheless, it is often difficult for families, especially among culturally and economically diverse populations, to access appropriate services, which ultimately impedes the long-term success of these children6 and substantially increases the lifetime cost of care7-8. This commentary provides an examination of the Pathways Early Autism Intervention (Pathways), a translational parent-mediated intervention for toddlers with ASD. Pathways fits the service delivery model and principles of Texas’ state-funded Early Childhood Intervention (ECI) programs and has been found to be effective with culturally and economically diverse families. Programs such as Pathways when implemented within ECI programs can help states offer cost-effective services, build capacity for their early evidence-based interventions, and break down barriers to timely intervention.
Best practices for toddlers with ASD
There is now sufficient evidence to suggest that best practice for toddler-aged children with ASD involves parents’ being coached to incorporate specific developmental and behavioral strategies into naturalistic interactions9-16. Naturalistic developmental behavioral intervention (NDBI) models are now considered state of the art for treating toddlers with ASD15. This approach blends developmental, social pragmatic strategies with applied behavior analysis (ABA) techniques to address the core symptoms of ASD. Parents are encouraged to utilize daily routines and activities and embed intervention strategies throughout much of the toddlers’ day to promote participation and learning in an authentic setting4,5,13,16,17. Parent-mediated NDBI for toddlers differs from NDBI and ABA models for children older than 36 months that take place in homes, clinics, or classrooms, one-to-one with a therapist, for 20 to 40 hours a week15. Parent-mediated interventions require fewer professional service hours because professionals work with and support family members in regard to how to engage the toddler with ASD in meaningful family activities and daily routines,14,16 thereby providing the intensity of service delivery recommended by the National Research Council (2001)18.
Parent-mediated ASD interventions can be delivered in a manner consistent with the Individuals with Disabilities Education Act (IDEA), Part C Early Childhood Intervention (ECI) programs,12,14 IDEA Part C is a federal grant program that assists states in operating state-wide programs for infants and toddlers with disabilities. These ECI programs necessitate the provision of a family-centered intervention that enhances the family’s capacity to promote the child’s development within the child’s natural environment14,19. Thus, early autism intervention programs that can be implemented within IDEA Part C programs, can break down barriers by providing timely autism intervention to these vulnerable toddlers14.
Early ASD intervention as differing from general developmental interventions
It is noteworthy that ECI for toddlers with ASD differs from the general developmental ECI that is effective for other groups of children4,20. General developmental ECI often focuses on the development of words to request and label pictures or objects and increases the child’s utterance length without regard to a child’s early social and communication capabilities. Such linguistically based approaches do not provide the social environment necessary to develop the social relatedness and reciprocal social interaction that are core deficits in ASD20. Optimal outcomes for toddlers with ASD are realized when early intervention focuses on core social and communication features of ASD15,21 by targeting foundational social communication skills, such as face-to-face reciprocal social interactions,4,9,12,20 that are precursors to social understanding22-24.
The Pathways solution
There are a growing number of parent-mediated NDBI programs for ASD that address social and communication skills10,14,16,25. Recently, Rollins and colleagues12,20,26 evaluated the efficacy of the Pathways program, a manualized parent-mediated NDBI for toddlers with ASD. Pathways was developed for use in IDEA Part C programs to facilitate access to timely and appropriate treatment for toddlers with ASD. Pathways’ interventionists made weekly visits to the toddler’s home and coached the caregiver for 90 minutes, as schedules permitted. The program includes parent coaching on an innovative protocol that works directly on socially engaged eye contact. Other NDBI toddler programs use interactional strategies similar to those of Pathways (e.g., face-to-face reciprocal interactions, animation, imitation) but do not work directly on social eye gaze (Table 1)4,9,13,16. The importance of facilitating social eye gaze as an intervention target has been emphasized by Jones and Klin,28 who found that, despite the presence of early reflexive gaze to adult eyes, infants with ASD exhibit a decline in eye gaze between the ages of 2 and 6 months. Their findings suggest that typical social interactions get derailed early in development and that intervention that focuses specifically on social eye gaze may adjust the pattern of brain activity toward a more typical trajectory20,28,29.
Table 1. Comparison of Key Components of Intervention
| Pathways NBDI | Other NBDI |
|---|---|
| Follow child’s lead, limit distractions, use wait time | Follow child’s lead, limit distractions, use wait times |
| Face-to-face dyadic interactions and social sensory routines | Face-to-face dyadic interactions and social sensory routines |
| Immediate and consistent reinforcement of activities and behaviors | Immediate and consistent reinforcement of activities and behaviors |
| Facilitation of social eye contact without aversive prompts | Facilitation of communication (requesting action and object, naming objects) |
| Use of animation | Use of animation |
| Imitation of the child | Imitation of the child |
| Facilitation of imitation; modeling and expansion of language | Facilitation of imitation; modeling and expansion of language |
Participants in the Pathways efficacy studies were recruited through local ECI programs and community centers. Eligibility criteria included (a) being less than 36 months of age at the start of the study; (b) meeting the criteria of the Autism Diagnostic Observation Schedule-2 (ADOS-2)30 for ASD and receiving a research diagnosis by an expert clinician; (c) having no other medical, neurological, or genetic concerns or disorders; and (d) the primary language of the home’s being English or Spanish.
In each of the studies reviewed below, caregiver-child dyads were digitally recorded for 10 minutes, using an iPad for a wide-angle recording of the interaction (Video Stream 1) and using hidden camera eyeglasses worn by the parent to capture the child’s eye contact (Video Stream 2). For each recording, the two streams of digitized videos (i.e., iPad and glasses) were segmented into 2- to 5-second intervals, depending on the study, and time-linked for partial interval coding. Outcome measures were social eye gaze (i.e., the number of intervals in which the child smiled while simultaneously looking at the parent’s eyes), vocal/verbal reciprocity (i.e., the number of intervals in which the child took at least one vocal or verbal turn, following the parent’s initiation). Diversity of communication acts were coded using the Inventory of Communicative Acts-Abridged (INCA-A)31. Inter-rater reliability, expressed as Cohen’s kappa, was high across all coded measures in each study.
Pathways Phase 1 studies
Using a single-subject multiple baseline across participants design with four culturally diverse toddlers enrolled in an IDEA Part C program, Rollins and colleages12 found Pathways to be an effective intervention for developing the early foundational social communication skills of social eye gaze and verbal reciprocity. Intervention effectiveness was measured by visual inspection and by percentage of non-overlapping (PND) data points from the baseline phase to the intervention phase. PND ranged from 78-100% in at least three children meeting the criteria for moderate-to-high effectiveness12.
Social validity showed a high level of satisfaction, as parents perceived the intervention as beneficial, easy to learn, and easy to incorporate into daily life. Prior to the start of the study, all toddlers received general developmental ECI services, which focused on generic developmental outcomes, for an average of five hours a month for 9.5 months. Despite the substantial expenditure of time and money, the data from the baseline phase suggest that the toddlers’ ECI services resulted in little progress toward remediating the core symptoms of autism.
These results were supported by a second case study20. Again, the intervention was effective for social eye gaze, verbal reciprocity, and social communication outcomes. Further, a SensoMotoric Instruments (SMI) portable eye tracker was used to measure the change in social eye gaze at the beginning and end of five weeks of Pathways intervention. The data were collected while the child sat on his or her caregiver’s lap in front of a 15-inch LCD display. A video of a female actor who was looking directly into the camera, singing childhood songs to simulate a dyadic interaction, was presented on the laptop that ran SMI’s Experiment Center. The percentage of time that the child looked at the actor’s eyes increased from 11.4% at baseline to 41.4% at the end of the intervention. The latter percentage was remarkably similar to the percentage of time that a typically-developing child, matched on age (29 months), mother’s age (34 years), and language in the home (English), looked at the eyes of the actor in the video.
Pathways randomized control trial
In a more recent study, 34 culturally and socioeconomically diverse toddlers with suspected or confirmed ASD were randomized into a Pathways group, a parent-mediated NDBI that worked on communication rather than shared eye gaze (Table 1), or a business-as-usual (BAU) group26,27. The BAU group all attended IDEA Part C programs, although some of the children had their ECI supplemented with traditional ABA services. Of the children, 40% were Medicaid- or CHIP-eligible, which means that they qualified for free or heavily subsidized health care. In addition, a third of the sample were bilingual or monolingual Spanish. Spanish-speaking caregivers received a Spanish language manual, and the parents were coached in Spanish. A two-way mixed ANOVA tested response to treatment for the social communication variables. A significant group-by-time interaction found Pathways, with its protocol for social eye gaze, was more effective in facilitating performance in social eye gaze and on a standardized social scale (Vineland Adaptive Behavioral Scale32 social composite) as compared to the other two groups (partial η2 = .321 and .183 respectively; Figure 1)26,27. Further, a significant group-by-time interaction found both the Pathways and the NDBI groups were more effective than was the BAU group in facilitating verbal reciprocity (partial η2 = .195)26,27 and communication outcomes (partial η2 = .193)26.
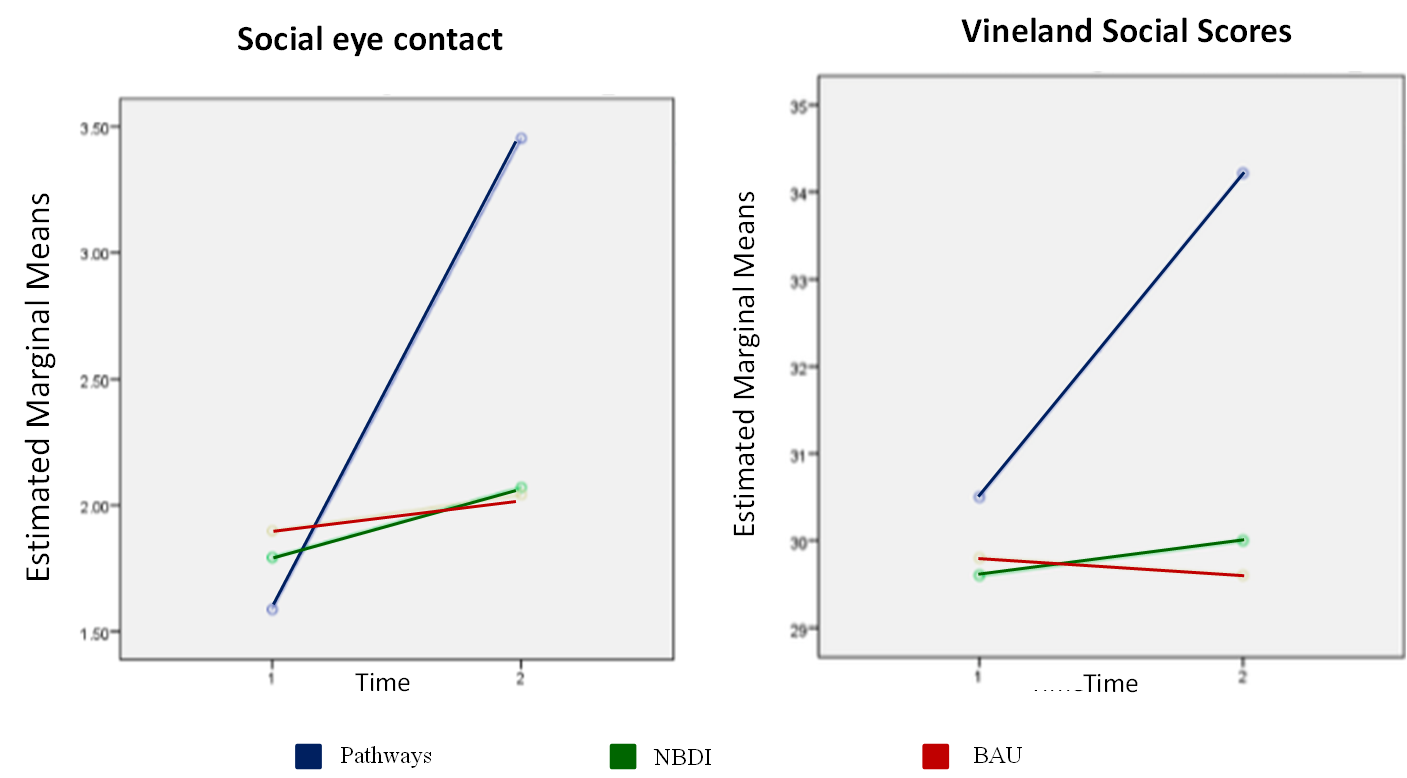
Figure 1: Graph of group-by-time interaction for the social eye gaze and Vineland raw scores
Dependent t-tests on pre- and post-parental stress scores, (measured by the Parents Stress Index-4 Short Form)33 found that both Pathways and the NBDI interventions had a medium effect on relieving parent stress (Cohn’s d=.43 and .58 respectively) where the BAU interventions had no effect on parental stress26.
It is noteworthy that the Pathways intervention involved coaching parents to facilitate social eye gaze and verbal-vocal reciprocity but did not involve coaching them on facilitating communication. Nonetheless, toddlers in the Pathways group made similar progress on communication outcomes as did the toddlers from the group that involved coaching parents on facilitating communication. This finding suggests that shared eye gaze may be a pivotal skill for the development of social skills and, when acquired, may have a cascading effect on social communication. Also noteworthy is that the BAU group, who were receiving ECI, made no progress in critical social and communication outcomes.
Discussion
The studies reviewed here corroborate the necessity for IDEA Part C programs to implement ASD-specific intervention such as Pathways. Pathways employs a 90-minute per week parent coaching model that can be adopted by IDEA Part C providers. Noteworthy was the finding that children in the control conditions (baseline phase or the BAU group) made little progress toward social relatedness despite having received at least an equal number of hours of intervention each week. Toddlers in the control conditions received ECI services that focused on the development of vocabulary to request, label pictures or objects, and increase the toddler’s utterance length without regard to the toddlers’ early social capabilities. These children may have made gains in areas not addressed in this study; however, they did not make gains in the early foundational social and communication outcomes that are known to be important contributing factors to an optimal outcome in toddlers with ASD21.
The symptoms of ASD can cause parent stress and interfere with family relationships, learning, and development, all of which affect a child’s long-term outcomes. Despite there being no cure for ASD, early identification and ASD-specific intervention that focuses on core social deficits are imperative for these children to be able to reach their optimal potential2,3,5,20. Many ASD intervention services are extremely costly and are accessible mainly to the privileged few. Identifying NDBI programs that can be implemented in publicly funded IDEA Part C programs that are accountable for reaching traditionally underserved populations is greatly needed. The studies reviewed here found Pathways to provide the intensity of services necessary for change in foundational social communication skills that are precursors to social understanding. Pathways shows promise as an effective focused NDBI that targets core social deficits of ASD, reduces parental stress and has the potential of being implemented within publicly funded ECI programs.
Acknowledgments
The research reported here was supported by a grant from the Texas Higher Education Coordinating Board’s Autism Grants Program and a grant from the Texas Department of Aging and Disability Services, in conjunction with the Texas Council on Autism & PDD and the Texas Autism Research and Resource Center.
Conflicts
There are no conflicts of interest to declare.
References
- Centers for Disease Control and Prevention. Facts about ASDs. 2014. Available from http://www.cdc.gov/ncbddd/autism/data.html
- Dawson G, Rogers S, Munson J, et al. Randomized, controlled trial of an intervention for toddlers with autism: the Early Start Denver Model. Pediatrics. 2010; 125(1): e17–e23.
- Reichow B. Overview of meta-analyses on early intensive behavioral intervention for young children with autism spectrum disorders. J Autism Dev Disord. 2012; 42(4): 512–520.
- Wallace KS, Rogers SJ. Intervening in infancy: implications for autism spectrum disorders. J Child Psychol Psyc. 2010; 51(12): 1300–1320.
- Warren Z, Mcpheeters ML, Sathe N, et al. A systematic review of early intensive intervention for autism spectrum disorders. Pediatrics. 2010; 127(5): e1303–e1311.
- Thomas KC, Ellis AR, McLaurin C, et al. Access to care for autism-related services. J Autism Dev Disord. 2007; 37(10): 1902–1912.
- Jacobson JW, Mulick JA. System and cost research issues in treatments for people with autistic disorders. J Autism Dev Disord. 2000; 30: 585–593.
- Stahmer AC, Brookman L, Frazee K, et al. Parent and multidisciplinary provider perspectives on earliest intervention for children at risk for autism spectrum disorders. Infant Young Child. 2011; 24(4): 344–363.
- Ingersoll B, Gergans S. The effect of a parent-implemented imitation intervention on spontaneous imitation skills in young children with autism. Res Dev Disabil. 2007; 28(2): 163–175.
- Kasari C, Gulsrud AC, Wong C, et al. Randomized controlled caregiver mediated joint engagement intervention for toddlers with autism. J Autism Dev Disord. 2010; 40(9): 1045–1056.
- Rogers SJ, Estes A, Lord C, et al. Effects of a brief Early Start Denver Model (ESDM)-based parent intervention on toddlers at risk for autism spectrum disorders: a randomized controlled trial. J Am Acad Child Psy. 2010; 51(10): 1052–1065.
- Rollins PR, Campbell M, Hoffman RT, et al. A community-based early intervention program for toddlers with autism spectrum disorders. Autism: The International Journal of Research and Practice. 2016; 20(2): 219–232.
- Schertz HH, Odom S. Promoting joint attention in toddlers with autism: a parent-mediated developmental model. J Autism Dev Disord. 2007; 37(8): 1562–1575.
- Schertz HH, Baker C, Hurwitz S, et al. Principles of early intervention reflected in toddler research in autism spectrum disorders. Top Early Child Spec. 2011; 31(1): 4–21.
- Schreibman L, Dawson G, Stahmer AC, et al. Naturalistic developmental behavioral interventions: empirically validated treatments for autism spectrum disorder. J Autism Dev Disord. 2015; 45(8): 2411–2428.
- Wetherby AM, Woods JJ. Early social interaction project for children with autism spectrum disorders beginning in the second year of life: a preliminary study. Top Early Child Spec. 2006; 26(2): 67–82.
- Diggle T, McConachie H, Randle V. Parent-mediated early intervention for young children with autism spectrum disorder. Cochrane DB Syst Rev. 2002; 2: 1–30.
- National Research Council. Educating children with autism. Washington, DC: National Academy Press; 2001.
- Adams RC, Tapia C. Early intervention, IDEA Part C services, and the medical home: collaboration for best practice and best outcomes. Pediatrics. 2013; 132(4): e1073–e1088.
- Rollins PR. Words are not enough. Top Lang Disord. 2016; 36(3): 198–216.
- Anagnostou E, Jones N, Huerta M, et al. Measuring social communication behaviors as a treatment endpoint in individuals with autism spectrum disorder. Autism. 2015; 19(5): 622–636.
- Adamson K, Russell C. Emotion regulation and the emergence of joint attention. In P. Rochat (Ed.), Early social cognition: understanding others in the first months of life (pp. 281–295). Mahwah, NJ: Lawrence Erlbaum; 1999.
- Greenspan SL, Shanker S. The role of affect in language development. Theoria. 2005; 54: 329–343.
- Rollins PR, Greenwald L. Affect attunement during mother-infant interaction: how specific intensities predict the stability of infants’ joint attention. Imagination, Cognition and Personality. 2013; 32(4): 339–366.
- Brian JA, Smith IM, Zwaigenbaum L, et al. Cross-site randomized control trial of the Social ABCs caregiver?mediated intervention for toddlers with autism spectrum disorder. Autism Res. 2017; 10(10): 1700–1711.
- Rollins PR. Creating a social pragmatic environment for toddlers with ASD and their caregivers. Talk presented at: The Friday Language and Speech, Hearing Series (F.L.A.S.H.), at the UT Dallas Callier Center; October 2017; Dallas, TX.
- Rollins,PR. Setting the Stage: Creating a Social Pragmatic Environment for Toddlers with ASD and Their Caregivers. Revista De Logopedia, Foniatria y Audiologia. (in press).
- Jones W, Klin A. Attention to eyes is present but in decline in 2–6-month-old infants later diagnosed with autism. Nature. 2013; 504: 427-31.10.1038/nature12715
- Dawson G, Jones EJ, Merkle K, et al. Early behavioral intervention is associated with normalized brain activity in young children with autism. J Am Acad Child Psy. 2012; 51(11): 1150–1159.
- Lord C, Rutter M, DiLavore PC, et al. Autism Diagnostic Observation Schedule: ADOS-2. Los Angeles, CA: Western Psychological Services; 2012.
- Ninio A, Snow CE, Pan BA, et al. Classifying communicative acts in children’s interactions. J Commun Disord. 1994; 27(2): 157–187.
- Sparrow SS, Cicchetti DV, Balla DA. Vineland Adaptive Behavior Scales (2nd ed.). Minneapolis, MN: NCS Pearson; 2005. Abidin RR. Parents Stress Index, third edition professional manual, Lutz, FL: PAR; 1995.
